The pigmented changes in the eye protein arise from pigment cells (melanocytes and melanophores). They produce melanin that protects the body against excessive ultraviolet radiation. Unfortunately, however, these changes can also initiate benign or malignant disease. Of course, race-related melanosis also occurs in non-Caucasian people. It is a brown, brownish-yellow or brown-black color within the palpebral fissure, most intense at the corneal limbus. A spot on the white of the eye – what does it actually mean?
A spot on the white of the eye – symptoms
In fact, everything from minor injuries to cancer can cause spots in the whites of the eye. Obviously, most spots are not serious and occur without any additional symptoms. However, if you notice a change in the protein of the eye, it is always worth visiting an optometrist.
The eye is filled with a sticky protein gel that gives the shape of the eyeball. The gel makes up about two-thirds of the eye’s volume and is mostly water. In early life, the protein is thicker, it has the consistency of egg white. With age, it begins to thin out and become more fluid. As the protein becomes more fluid, small pieces pull away from the retina.
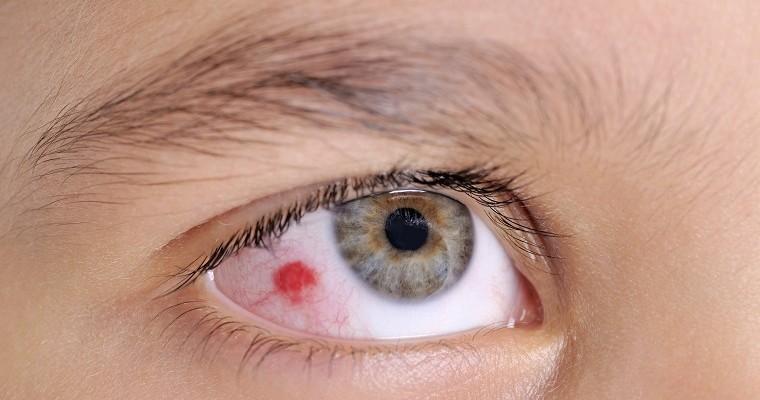
Sometimes the appearance of plaque and redness in the cornea of the eye is caused by the use of eye drops containing vitamin C. In contrast, Horner-Trantas dots are characterized by small rounded bumps, called papillae, on the surface of the eye or eyelid. Additional symptoms include severe itching, photophobia, foreign body sensation, discharge, eyelid spasm, and blurred vision. As for moles that appear around the iris or under the retina, they are often harmless, but can also develop into eye cancer.
Pinguecula is the conjunctival compaction. This lesion is not cancerous, it appears as lumps on the eyeball, at the top of the middle sclera. It is caused by exposure to ultraviolet radiation and frequent exposure to dust and wind. It often affects elderly people who spend a lot of time outside without sunglasses or a hat.
Pterygium is the fleshy tissue on the conjunctiva. It forms on the side of the nose and may grow towards the pupil. Despite its disturbing appearance, pterygium is not cancerous and its growth usually slows down over time or stops. In extreme cases, the pupil is partially or completely covered and causes visual disturbances.
Racial melanosis is a mild disease. It is characterized by flat conjunctival pigmentation or dark spots. The condition rarely develops into conjunctival melanoma.
The cause of the macula will determine what kinds of complications can develop. For the most part, however, stains on the white of the eye do not have serious complications, but there may be excessive itching. However, depending on the cause of the macular occurrence, it can cause significant discomfort, leave scarring and even develop into cancer. Only after the doctor determines the cause of the change that appears in the white of the eye, the appropriate treatment can be adjusted.
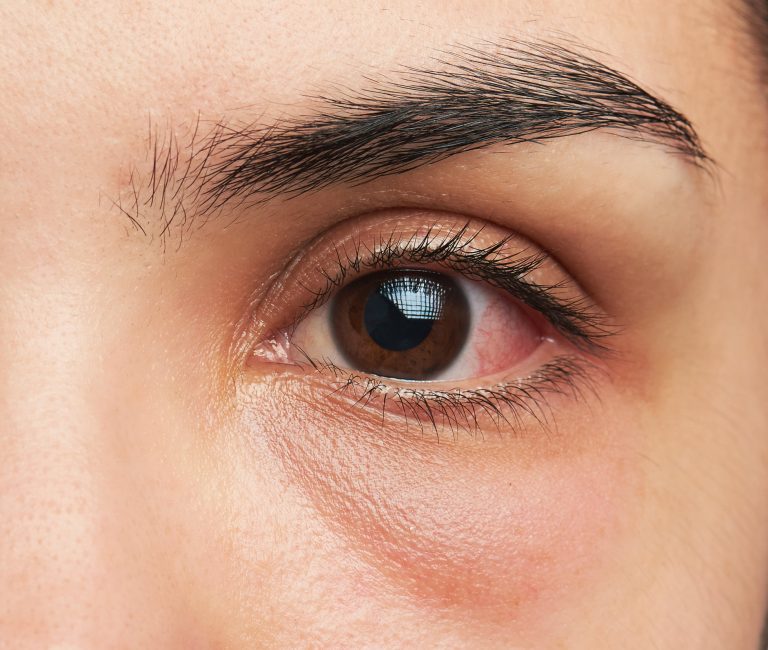
Black spot on the white of the eye
The appearance of a black spot on the white of the eye is usually just a pigmented lesion of the protein conjunctiva and must be examined by a doctor.
Stains can come in various forms – you may notice black, brown, red or yellow colors. In some cases they are harmless, in others they may require more comprehensive treatment. If you notice changes, make an appointment with an optometrist. Most often, such changes need to be monitored regularly.
You may also find that under certain conditions – bright light, for example – you will notice a dark spot in your field of vision. This is the phenomenon of so-called floaters or floaters. They are usually caused by changes in the gel in the eye and appear with age. Stains can be seen as the undissolved gel particles diverge and float in the liquid protein. The shadows they cast on the retina cause visible stains that you may notice especially in bright light or when you look at a lit screen.
Visible spots in the eye can also be the result of a small blood vessel rupture. This can be caused by many different factors, including lifting particularly heavy objects or trauma to the eye area. In some cases, visible spots under the eyes may also indicate other diseases, such as diabetes or high blood pressure.
In some cases, the optometrist may prescribe medications. Occasionally, your doctor may refer you to a doctor for further screening tests or recommend surgery to correct any eye problems before your eyesight is affected. Sometimes “floaters” can be a symptom of a disconnected retina, requiring immediate surgery.
Dark spots on the white of the eye
The appearance of dark spots is usually a pigmented nevus known as melanin. It requires observation, and if it changes, it is necessary to visit an ophthalmologist. Sometimes such spots can be removed surgically, but it is recommended to leave them as the procedure may cause unnecessary complications. Unfortunately, the causes of the development of pigmentary changes in the conjunctiva are not fully understood. Some of the pigment cells accumulate excessively in one place during development. There are cases where the number of pigment cells in a given site is normal, but there is an excessive amount of pigment in them.
In conjunctival melanoma, the melanocytes can turn into cancerous cells when exposed to sunlight. This cancer is rarer than skin melanoma or intraocular melanoma, and it is less common in people from Africa and Asia.
A dot on the white of the eye
A red spot in the eye is a sign of a rupture of a blood vessel. Although it does not have any serious consequences, it is worth visiting an ophthalmologist, as it is sometimes one of the symptoms of subconjunctival hemorrhage or serious diseases.
However, if the red spot is not associated with any diseases, it is spontaneously absorbed usually after 10-14 days. Sometimes a blood vessel in the white of the eye ruptures and a spot appears in people who use poorly selected contact lenses. Inadequate lenses cause abrasions to the corneal epithelium and make it difficult to exchange fluids under the lens. Too tight contact lenses cause burning and stinging, irritation of the limbus or conjunctiva vessels. Subconjunctival haemorrhage, on the other hand, means that lenses are worn too long. It also happens that the appearance of a red spot is the result of an excessively dry eye. The reason for this is too much time spent in front of the computer or in air-conditioned rooms. Often additional symptoms of dry eye are burning pain and sensitivity to light.
Subconjunctival hemorrhage is often the result of eye irritation. A red spot in the eye can also be caused by overexertion, coughing, sneezing, vomiting, constipation, or laughing.
Sometimes the red spot is caused by the wrong treatment for diabetes or atherosclerosis. Diabetes has a negative effect on the condition of the blood vessels in the eyes, and can lead to retinopathy, i.e. damage to the retina. Atherosclerosis, in turn, makes blood vessels brittle and prone to rupture.
The red spot may also be caused by a sudden increase in blood pressure, and may also appear when taking acetylsalicylic acid, such as aspirin or polopyrin, and when taking non-steroidal anti-inflammatory drugs that lead to bleeding. Subconjunctival hemorrhage can also be caused by blood clotting disorders as well as vitamin K deficiency.
Hormonal disorders also affect the breaking of blood vessels. During pregnancy, red spots on the protein and even deterioration of eyesight appear very often. After childbirth, symptoms disappear on their own.
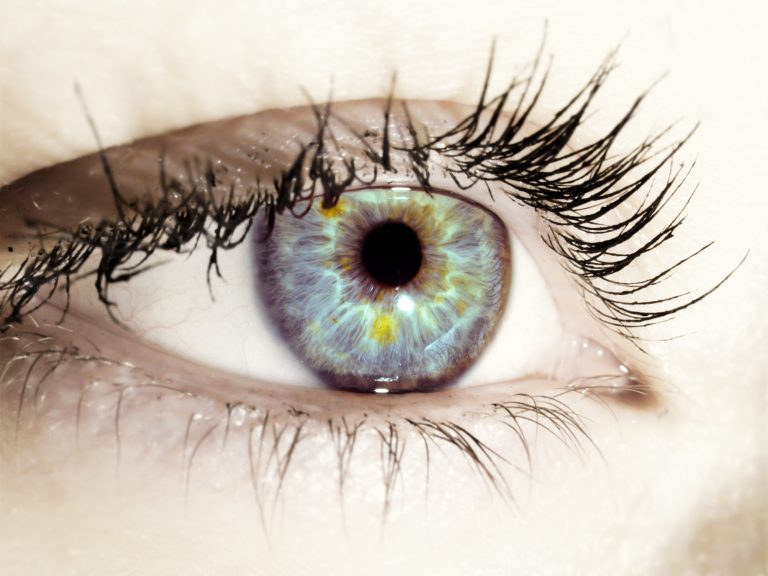
A spot on the white of the eye in a child
The appearance of a spot on the white of the eye in a child may be caused by the water vessel of the eye, pigmented spot or mechanical trauma. Even if the cause is known, the matter should not be underestimated and be sure to see a doctor and ophthalmologist, especially if the child has bright eyes.
A spot on the white of the eye – which means
Pigmented lesions are most often brown, brown-yellow, brown-gray, gray or black. Sometimes amelanotic changes, i.e. colorless, may be pink or yellow. They are also derived from melanocytes, but do not produce a pigment.
Many of these changes are not a threat. However, special attention should be paid to raised or atypically located changes. A visit to the doctor is necessary especially if the lesion takes a different shape, when the degree of dye saturation changes, and when new lesions or lumps appear.



